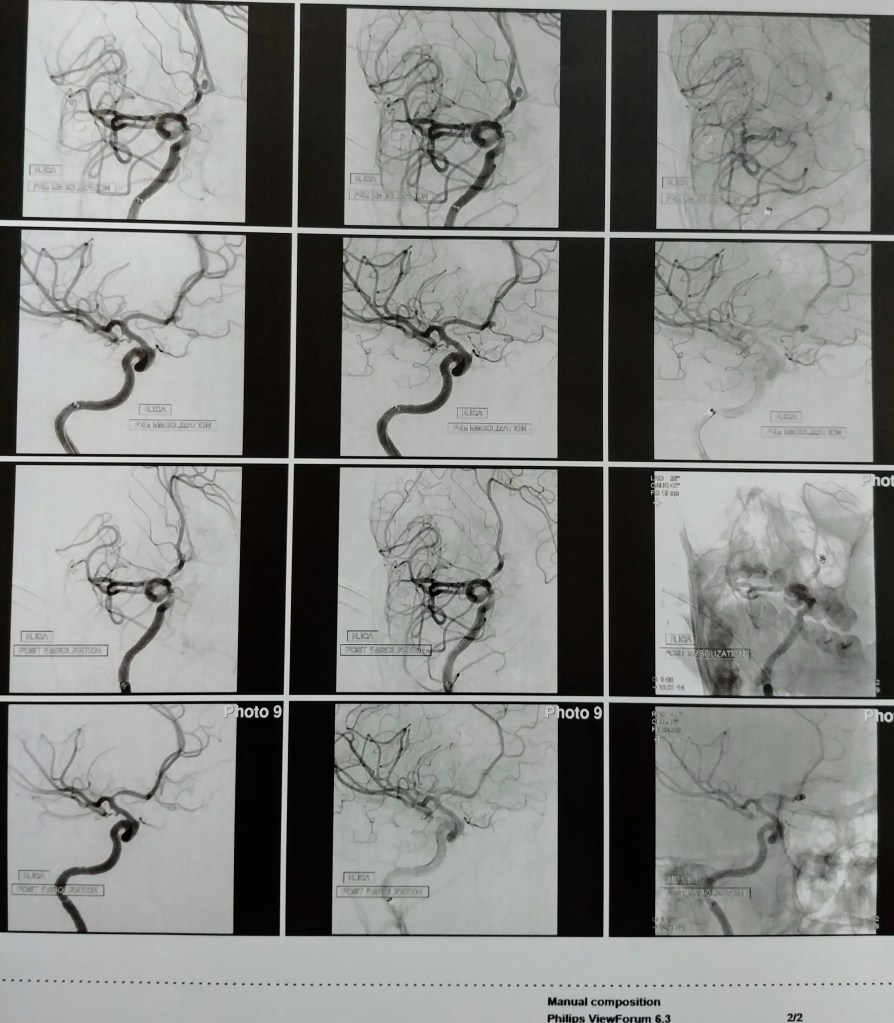
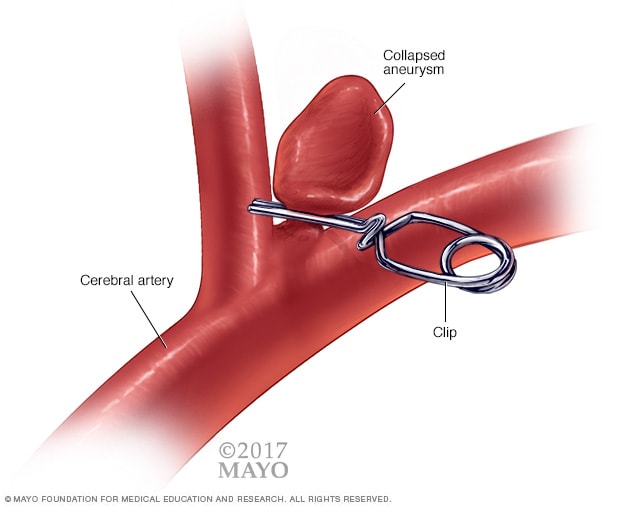
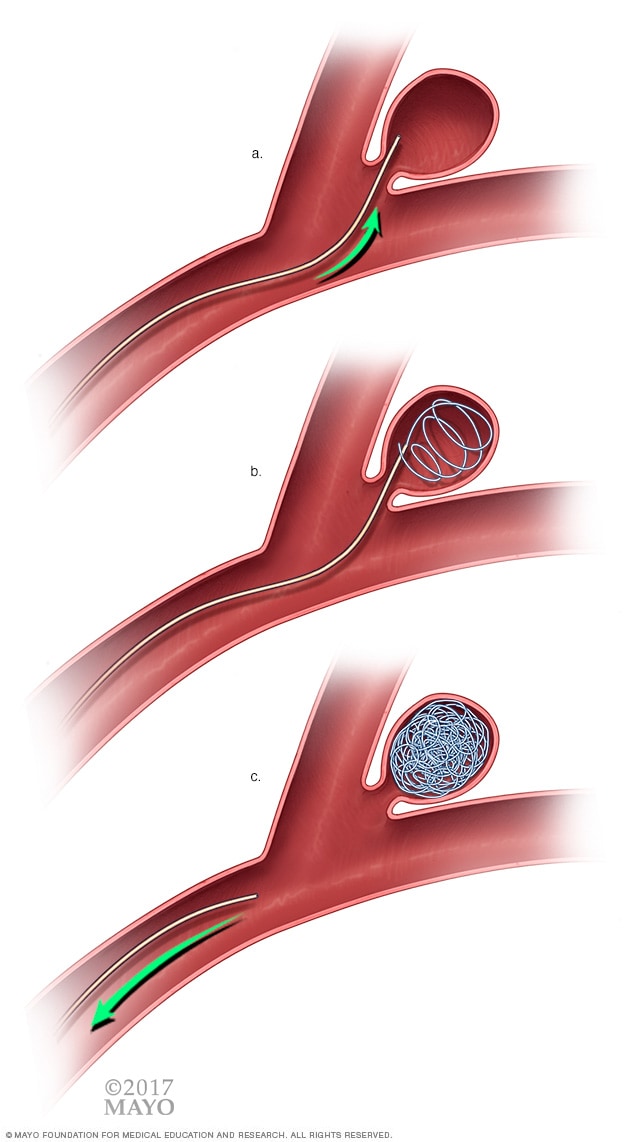
His story continues…
They decided to airlift you to Pretoria, South Africa, close enough to the medevac center for US Diplomats in the region. We all agreed that despite the risks involved with flying, it was the only best option to help save your life. AMREF air ambulance from Nairobi, Kenya, was organized and by 4pm on Saturday, about 15hours from when the aneurysm happened, you were on the tarmac in Entebbe airport ready to depart for South Africa.
The kids and I flew
separate on a commercial airline after the plan to go with you in the air
ambulance failed. We arrived in early Sunday morning and I had a lot of help
from the Embassy. They helped organize for nannies, transportation,
accommodation, and treatment for the kids.
You were send straight to Kloff Hospital where the neurosurgeons immediately started working on your case. Surgery was scheduled for Monday, August 1st. At that time, it was all up to God to guide everything. Almost all of the family members, friends, and relatives who were aware of your condition, were praying. Everything was being done by the hospital staff to keep you stable until the bleeding was stopped. I was anxious but hopeful.
The long awaited day came for the procedure to be done, I signed the papers and off they took you. I waited anxiously in the waiting room for the doctor to come out with good news. The procedure was to take 3-4hours. As I was gazing at the postings on the wall related to all types of aneurysms, the door opened and it was your neurosurgeon. It had only been 30minutes since they took you in. What could he be doing here right now? I asked myself as I starred at the disappointment look on his face. “Mr. Field, I am sorry to disappoint you, I know how anxious you are but things didn’t turn out the way we had planned. There has been a change of plan.” I don’t recall if I said anything to him or heard the rest of what he had to say. All I remember is feeling like somebody had just punched me right in the chest and removed my heart. I felt like I had stopped breathing. My whole body was shaking, my vision was blurry and my mind was blank all to the thought of having lost you. I must have fallen back or perhaps fainted but I recall the doctor calling a nurse to bring me some water and a cold wash cloth. After a few minutes, he explained to me that they had not lost me but rather cancelled the procedure after it was deemed to be more risky than previously assumed. He then added that he was going to consult with other neurosurgeons and the Embassy Doctor in order to come up with the safest yet most effective plan.
They brought you out of the surgery room looking a little bit drowsy from the anesthesia but still had your beautiful smile. I was so happy to see you even though I was dying inside from the anxiety. Your memory was still bad and you asked the same repetitive questions but every time I looked into your eyes, I saw hope, I saw life, I saw outstanding strength. One side of me was telling me that I shouldn’t sign the papers to give them authority to perform the procedure and accept all the complications, including death, which might occur. It was better to have you alive at that moment, bedridden, and confused than not to have you at all. I wished badly to freeze that moment in time because that was all I was sure of. The kids and I would wanted to see you and have your presence in our lives despite the disorientation. The thought of losing you especially after the procedure was stopped that day was impossible for me to accept and carry on with life. The other side of me was telling me to take the risk and have them do the procedure. Despite all the risks involved, somehow, I knew you were going to be fine. My heart was content with that decision. I tried to ask you what you wanted me to do but you were not able to answer. You did not respond to any questions that I asked other than the programed ones.
Later that day, the
neurosurgeon came in and told me that they were going to transfer you to
Netcare Unitas Hospital in Centurion where the other neurosurgeon would take
lead on carrying out the procedure the following day. At this point, time was
critical, every second was counting. The ambulance was organized and you were
transferred to the ICU unit in Unitas Hospital. I went back to the hotel to
organize for early checkout to another hotel that would be closer to Unitas
Hospital and relieve the nanny from her job. At this point, all the kids were
sick, the oldest one had refused to eat food insisting that he only wanted mama
to feed him. Luckily, there was one nanny who agreed to stay for almost a week
until your sister arrived. This nanny was so kind to the kids and was able to
gain trust from our son, who later agreed to take food from her. This allowed
me time to focus on you, the children’s medical needs, and my job.
The following day, I headed to the Hospital where you had been transferred to prepare for your procedure. I signed the documents as required and the two neurosurgeons together with the medical doctor informed me that after a careful review of the procedure, they decided to go ahead and do it using a different but safer approach. Both neurosurgeons were going to perform the coiling procedure. Well, that was enough to reassure me that God was in control and no matter what the outcome would be, the best available approach was being used. So, off you went. I kissed you softly and told you that I would see you shortly. You smiled back and that is all I needed.
Approximately three and
half hours later, the lead neurosurgeon came to me in the waiting area. He
seemed relaxed and content. Without wasting time, he told me “Mr. Field, your
wife should be out shortly, the procedure went very well and she is expected to
make full recovery in 2-8weeks but the memory should start improving as soon as
the anesthesia wears off.” Tears of joy were dripping down my cheeks as I
reached out to him and extended my gratitude. I was overjoyed, I wanted
everyone to know that you were okay, I could not stopping smiling and thanking
God. I did not mind waiting for an extra 30minutes while you were still in
recovery room because I knew you were alright.
It was not too long before they brought you out on the stretcher and we started making our way to your room. As soon as we entered the elevator, however, you started coughing uncontrollably that the nurse started paging for help. She rushed you into your room where we found a team of care providers waiting. The physiotherapy took the lead to stabilize you. Fortunately, she was able to stabile you within 30minutes. I think she gave you a breathing treatment and bumped up your oxygen supply. After that, you started to verbalize more but you still complained of a severe headache. The nurse requested that I leave so she could give you some pain medicine and allow you time to rest. So, I left with a heart filled with joy ready to go and deliver the good news to the kids and our loved ones who had all been praying tirelessly and waiting anxiously to hear about the outcome of the procedure.
When I returned in the
evening, you could talk to me, ask me different questions about the kids and
what had happened to you and how we ended up in South Africa. You were able to
follow a conversation although your memory, short term memory in particular,
was not as sharp as it used to be. When
I came back the following morning, however, you had improved a lot. The focus
was now on your recovery.