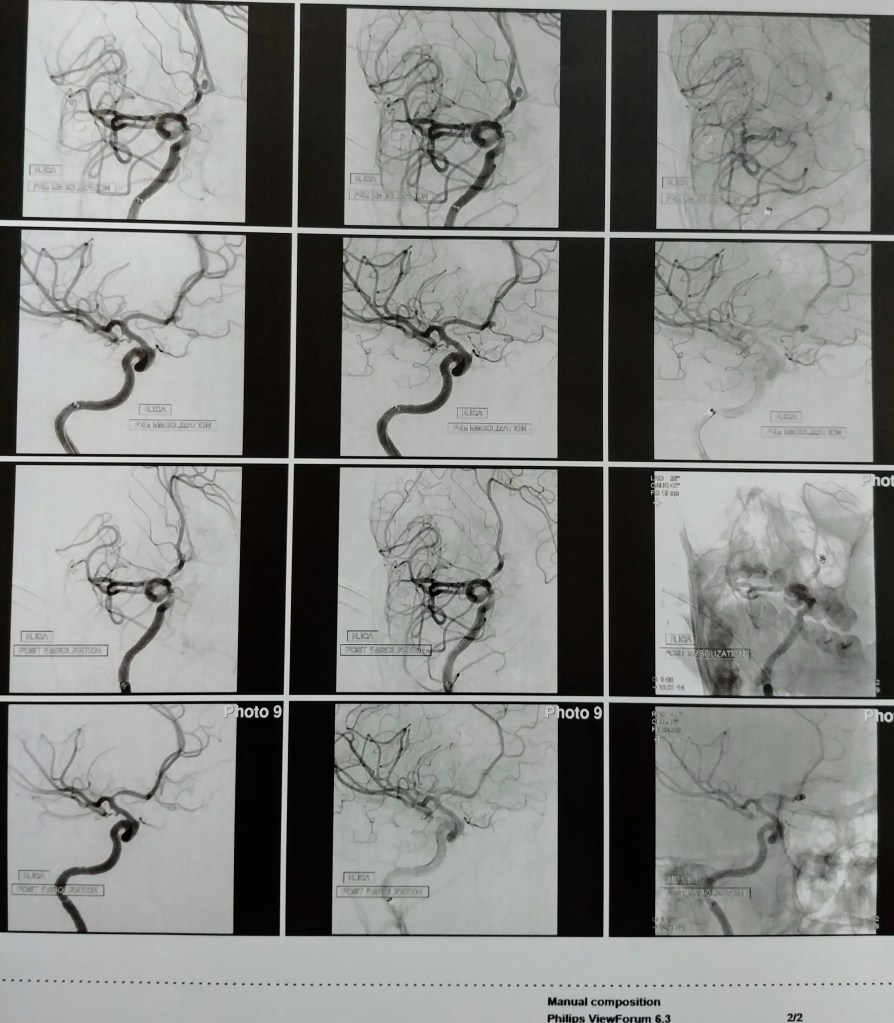
Brain aneurysms/cerebral aneurysms form when the walls of the arteries in the brain become thin and weaken. Aneurysms typically form at branch points in arteries because these sections are the weakest. Occasionally, cerebral aneurysms may be present from birth, usually resulting from an abnormality in an artery wall. Reference
Risk
factors for developing an aneurysm
Sometimes
cerebral aneurysms are the result of inherited risk factors, including:
- genetic
connective tissue disorders that weaken artery walls
- polycystic
kidney disease (in which numerous cysts form in the kidneys)
- arteriovenous malformations (snarled
tangles of arteries and veins in the brain that disrupt blood flow. Some
AVMs develop sporadically, or on their own.)
- history
of aneurysm in a first-degree family member (child, sibling, or parent).
Other
risk factors develop over time and include:
- untreated
high blood pressure
- cigarette
smoking
- drug
abuse, especially cocaine or amphetamines, which raise blood pressure to
dangerous levels. Intravenous drug abuse is a cause of infectious mycotic
aneurysms.
- age
over 40.
Less
common risk factors include:
- head
trauma
- brain
tumor
- infection
in the arterial wall (mycotic aneurysm).
Additionally,
high blood pressure, cigarette smoking, diabetes, and high cholesterol puts one
at risk of atherosclerosis (a blood vessel disease in which fats build up on
the inside of artery walls), which can increase the risk of developing a
fusiform aneurysm.
Risk
factors for an aneurysm to rupture
Not all
aneurysms will rupture. Aneurysm characteristics such as size, location,
and growth during follow-up evaluation may affect the risk that an aneurysm
will rupture. In addition, medical conditions may influence aneurysm rupture.
Risk
factors include:
- Smoking.
Smoking is linked to both the development and rupture of cerebral aneurysms.
Smoking may even cause multiple aneurysms to form in the brain.
- High
blood pressure. High blood pressure damages and weakens arteries, making
them more likely to form and to rupture.
- Size.
The largest aneurysms are the ones most likely to rupture in a person who
previously did not show symptoms.
- Location.
Aneurysms located on the posterior communicating arteries (a pair of arteries
in the back part of the brain) and possibly those on the anterior communicating
artery (a single artery in the front of the brain) have a higher risk of
rupturing than those at other locations in the brain.
- Growth.
Aneurysms that grow, even if they are small, are at increased risk of rupture.
- Family
history. A family history of aneurysm rupture suggests a higher
risk of rupture for aneurysms detected in family members.
- The
greatest risk occurs in individuals with multiple aneurysms who have already
suffered a previous rupture or sentinel bleed.
For my case, I had been diagnosed
with high blood pressure in the first trimester of my second pregnancy and the
condition was being managed when I suffered the brain aneurysm. No family
history of brain aneurysms that I am aware of. No smoking, no alcohol abuse,
and absolutely no drug use except for the ones for BP and vitamins. My take
from this is that we are all pretty much at risk. I have heard stories of
completely healthy people, very athletic, and with no family history get them. The
more information we know about brain aneurysms, the more lives we can help
save.